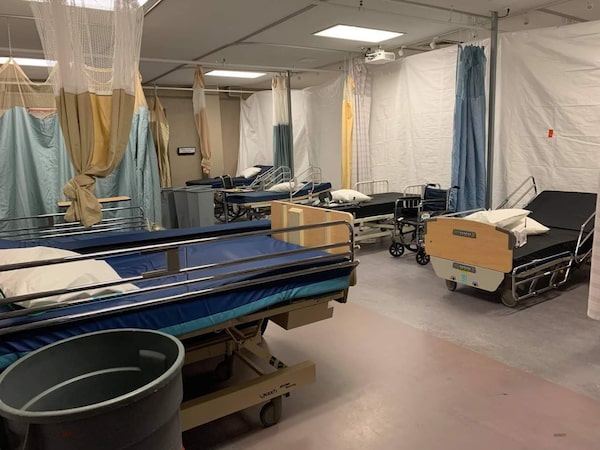
Sainte-Dorothee nursing home's 'hot zone,' an area set up for residents who tested positive. A nurse testified that it was 'dreadful, like a horror movie,' with people suffering from breathing problems lying next to dead residents.GAGN12/Handout
Pandemic medical rules that made it harder to hospitalize nursing home residents were death sentences for elderly people, a man who lost his 94-year-old mother told a coroner’s inquest Thursday.
“They condemned her, gave her morphine and two other drugs, then left her there, without assistance. … That’s the reason for my anger, for her and for all the others who died,” Jean-Pierre Daubois said in a testimony that was at turns angry and tearful.
At the start of the pandemic, Quebec focused on preparing hospitals for the crisis. Hospitals offloaded patients to long-term care facilities. Families of nursing home residents were asked to revise the care levels of their loved ones to favour end-of-life comfort care, rather than treatment to prolong life.
As a result, the inquiry has heard that families of residents at the Sainte-Dorothée nursing home struggled to get their ailing relatives to hospitals and many died instead at the home while sedated with morphine.
Quebec nursing home often gave morphine rather than treat COVID-19 patients, inquest told
Witnesses who followed Mr. Daubois on Thursday described the disarray and anguish that swept through Sainte-Dorothée, a home in Laval, north of Montreal, where 102 residents died during the first wave of COVID-19.
The inquest heard that three employees started to feel ill but had to keep working. “That made no sense,” a nurse testified.
The nurse, who worked in a physical rehabilitation unit called UTRF, was sent to the “hot zone,” a makeshift ward for residents who tested positive for the disease, or those suspected of being infected.
“The beds weren’t separated by much. There were no sinks. People moved from one patient to another without being able to wash their hands,” the UTRF nurse testified. (Her name and those of other staffers can’t be disclosed because of a publication ban.)
She said funeral homes were slow to show up. “There were dead people next to others who were in respiratory distress. They had bodies next to them. It was dreadful. Like a horror movie.”
The chaos in nursing homes happened after Quebec health authorities incorrectly expected that the novel coronavirus would hit hospitals first. “We expected very sick travellers in emergency wards,” testified Maude Saint-Jean, head of microbiology for Laval’s local health authority.
Officials also hadn’t yet grasped how the virus could be transmitted, Dr. Saint-Jean said.
She recalled that one orderly at Sainte-Dorothée wasn’t feeling well but was told to keep working because he didn’t show symptoms associated with COVID-19, such as coughing or fever. It was days later that they realized his loss of smell was a sign of the new disease.
The UTRF nurse said she worked with an auxiliary nurse who had a headache and fever. Their supervisor insisted the auxiliary nurse should keep working because she could wear masks and gowns.
The auxiliary nurse then reported that she had lost her sense of smell. “I told her to leave, that I would take responsibility. So she left, she went to get tested and she was positive.”
Another auxiliary nurse, who testified Thursday, said another employee was also not feeling well, telling her “I can’t do it anymore.”
“She was exhausted. She wanted to leave but she had to carry on. That’s what she told me.”
The auxiliary nurse who testified was among those who regularly looked after Mr. Daubois’ mother, Anna José Maquet. She testified that, despite her age, Ms. Maquet was lucid and seemed to be well on April 2.
However, the next morning, Ms. Maquet gagged while drinking a liquid, then vomited when she tried to take her medications. Her regular nurse was sick with COVID-19, so the only staff on the floor were the auxiliary nurse and a nursing candidate.
The auxiliary nurse ran to another floor to find a nurse who could talk to a doctor on the phone. Ms. Maquet was then prescribed comfort care, a mix of morphine, with a tranquilizer and scopolamine to clear lung congestion. She died later in the evening.
She was tested for COVID-19, but the result was lost. Her family thinks she wasn’t infected. She previously had episodes where she had trouble swallowing and her son said the staff should have tried to treat her.
“They did nothing. Nothing,” he said.
In March, before the pandemic struck, the family had received a call from the nursing home asking to revise Ms. Maquet’s care level to C, where care comfort would be given rather than treatment to prolong her life.
“They called us and explained that transporting people of her age to hospital … it could be more traumatic than not,” Mr. Daubois testified.
“They didn’t twist my arm. They explained it in a way that made me agree. … If they had told me the rest, that they wouldn’t take my mother to hospital when she needed a ventilator … I wouldn’t have agreed to that. They never told me that part.”
Our Morning Update and Evening Update newsletters are written by Globe editors, giving you a concise summary of the day’s most important headlines. Sign up today.
 Tu Thanh Ha
Tu Thanh Ha