Natalia Worek and her fiancé, Jermaine DeCosta, feed their newborn son, Praise, at Mr. DaCosta's parents' home in Ancaster, Ont. Ms. Worek, a registered nurse, came down with COVID-19 in her third trimester.Galit Rodan/The Globe and Mail
When Natalia Worek tested positive for COVID-19 in early May, she was worried, but not terribly so.
The 31-year-old in Ancaster, Ont., knew of a few friends and acquaintances who had caught the coronavirus and recovered. She presumed her own battle would be just as easy.
The difference turned out to be her pregnancy, an underlying condition that put her at increased risk of developing a severe case. Women such as Ms. Worek are now the target of a vaccination push across Canada to protect as many mothers-to-be as possible.
Her COVID-19 symptoms began on April 28, five days after the Ontario government announced it would move pregnant women into the “highest risk” category in the vaccination rollout, making them eligible immediately. But even if she had rushed out for a shot on the day of the announcement, her immunity wouldn’t have been sufficient to protect her in time.
As it stood, Ms. Worek, who felt her risk of catching the coronavirus was low because she was working from home, was nervous about taking a new vaccine whose initial clinical trials excluded pregnant women.
She was slightly more than 32 weeks pregnant with her first child when the virus began spreading through the home she and her fiancé, Jermaine DeCosta, shared with his extended family. Six of the nine members of the household tested positive, including Mr. DeCosta’s 52-year-old sister who remains on ECMO, a type of life support one step up from a ventilator.
“I was scared because I had the exact same symptoms as my sister-in-law,” said Ms. Worek, a registered nurse by training. “But I was just – again – thinking, ‘I’m not going to get to that point. I’m 31.’”
Older Canadians should be getting their second vaccine doses, right now
The condemned: On becoming a first-time mom during the pandemic
Nonetheless, she and Mr. DeCosta decided to call an ambulance when she could no longer bear her exhaustion, relentless fever and shortness of breath. On the night of May 4, paramedics drove her to St. Joseph’s Healthcare in Hamilton, where a team of about a dozen physicians and nurses reviewed her case.
They recommended she be put under for an emergency C-section. Ms. Worek called Mr. DeCosta, who wasn’t allowed into the hospital. The call lasted less than a minute. “It was like, this is what’s happening: I’m having a C-section. I love you. I’m scared. Pray.”
Tests revealed her platelet count was dangerously low, meaning the surgical team could run into trouble stanching her bleeding. Before she was anesthetized, someone warned Ms. Worek that, in the worst-case scenario, she might lose her uterus. “I was like, oh my god,” she recalled. “What if I wake up and I can never have kids again?”
Doctors at a Hamilton hospital delivered Praise by emergency C-section, a potentially risky procedure for Ms. Worek given her low blood-platelet count.Galit Rodan/The Globe and Mail
The public-health messaging around COVID-19 vaccines for expectant mothers has evolved as quickly as the virus itself, making it a challenge for women to keep up.
In less than six months, Canadian public-health authorities and immunization experts have gone from warning that they didn’t have enough information to recommend COVID-19 vaccines in pregnancy to entreating pregnant women to get the shot as soon as possible.
Two major shifts have occurred since Health Canada approved the country’s first COVID-19 vaccines in December with a line in the instruction manuals that read, “the safety and efficacy of [the vaccines] in pregnant women have not yet been established.”
The first is that early observations from the worldwide immunization campaign suggest the new mRNA shots, made by Pfizer-BioNTech and Moderna, are safe in pregnancy, as many experts in women’s reproductive health predicted they would be based on experience with other vaccines.
(Canada’s provincial governments have stopped offering the AstraZeneca vaccine, which uses viral vector technology, as a first dose to all people because of the risk of a rare but serious blood-clotting disorder unrelated to pregnancy.)
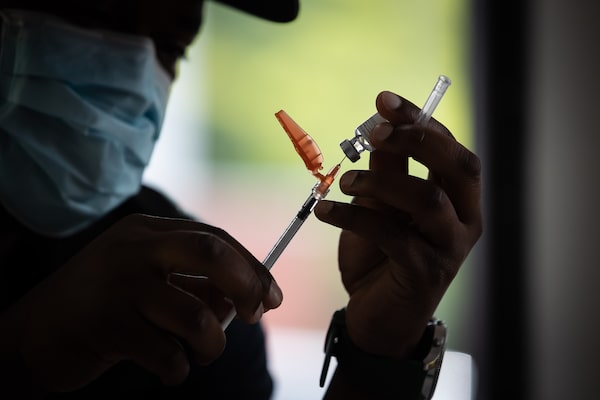
A registered nurse at B.C.'s Fraser Health region draws a dose of Pfizer at a walk-in clinic in Surrey, B.C.Darryl Dyck/The Canadian Press
Preliminary data from COVID-19 vaccine surveillance in the United States, published in late April in the New England Journal of Medicine, detected no red flags for pregnant women or their babies associated with receiving a COVID-19 vaccination in the third trimester.
In Canada, meanwhile, a pair of research teams funded by the federal government’s COVID-19 Immunity Task Force and Vaccine Surveillance Reference Group is monitoring women to further evaluate the safety and effectiveness of COVID-19 vaccines during pregnancy.
“To this day, there are no vaccines that have been shown to be dangerous in pregnancy,” said Deborah Money, a professor of obstetrics and gynecology at the University of British Columbia and a specialist in infectious diseases in pregnancy.
“Even the vaccines we avoid haven’t caused harm and the ones that we deliberately use have definitely shown benefit.”
Obstetricians generally say pregnant women shouldn’t take vaccines that use a weakened version of a live virus, such as the measles, mumps and rubella shot, but Dr. Money said the medical literature has never recorded an adverse outcome after a live vaccine was given inadvertently during pregnancy.
The main shots recommended in pregnancy – for whooping cough and the flu – have the added benefit of providing antibodies to infants who would otherwise be vulnerable to the viruses that cause both illnesses. COVID-19 vaccines given in pregnancy also protect newborns, early studies show.
A pregnant woman gets a dose of Sinovac's vaccine at a clinic in Apodaca, on the outskirts of Monterrey, Mexico.Daniel Becerril/Reuters
In a second significant shift since the vaccines were approved, public-health officials have come to better appreciate the threat COVID-19 poses to pregnant women.
CANCOVID-Preg, a Canadian surveillance effort led by Dr. Money, found that although the overall numbers were small, expectant mothers infected with the coronavirus were about five times more likely to be admitted to hospital or the intensive-care unit than women of reproductive age who weren’t pregnant, echoing data from elsewhere in the world.
“A pregnant individual uses more oxygen than a non-pregnant individual because they’re feeding both themselves and babe,” said Wendy Whittle, head of labour and delivery at Toronto’s Mount Sinai Hospital. “That just makes them incredibly vulnerable to any sort of infection that would target the respiratory tree.”
Detailed data from CANCOVID-Preg is only available up until the end of 2020, meaning it doesn’t capture the apex of Canada’s variant-fuelled third wave, which some front-line obstetricians, particularly in Ontario, say sent more infected pregnant women to hospital than previous waves.
For example, Mount Sinai, a referral centre for high-risk pregnancies, admitted 15 pregnant women with COVID-19 to the ICU in April and May, 2021, three times the number the hospital admitted to the ICU in the first year of the pandemic.
“[T]here is currently a daily wave of pregnant women and individuals coming into Ontario ICUs, many requiring ventilators. These women and individuals are getting extremely sick, very quickly,” the Society of Obstetricians and Gynaecologists of Canada said in a mid-April statement calling on governments to make pregnant women eligible for vaccines sooner.
Every province eventually heeded that call by moving expectant mothers up the queue or opening vaccine appointments to all ages.
“I always emphasize this: The majority of [pregnant women with COVID-19] will have mild to moderate disease,” said Susan Ellis, chief of obstetrics at St. Joseph’s Healthcare Hamilton. “But the reason we’re advocating for the vaccine, and the reason we’re more concerned in wave three, is that the people who develop severe disease are people we wouldn’t necessarily have been able to predict because of other risk factors.”
In other words, some are healthy young mothers-to-be such as Ms. Worek.
Between late April and early May, Ms. Worek was one of three pregnant women with COVID-19 to give birth by emergency C-section at the same hospital in Hamilton.Galit Rodan/The Globe and Mail
Ms. Worek has no memory of the day after her son, Praise, was born, weighing less than 4 1/2 pounds. It was May 5 and she was in the ICU, recovering from a successful C-section that did not end with a hysterectomy.
Still contagious, Ms. Worek was only allowed to see her baby from the window of her room in the COVID-19 ward at St. Joseph’s. By fluke, nurses on the COVID-19 floor had discovered that rooms 485 and 486 overlooked the third-floor special-care nursery in an adjacent wing of the hospital.
A week after Praise was born, Ms. Worek met him for the first time. Hospital staff lined the halls and clapped as she was pushed in a wheelchair from the COVID-19 floor to the special-care nursery. A staff member made posters with Praise’s picture declaring, ‘I can’t wait to meet you.’”
Ms. Worek was one of three pregnant women with COVID-19 who had emergency C-sections after being rushed to St. Joseph’s by ambulance in late April and early May. All spent part of their isolation and recovery period in the rooms with a view of the nursery, waving as nurses held their infants up to the glass.
Trisha Mayer, 38, found herself in room 485 a few days after Ms. Worek. She gave birth to Isaac, her sixth child, on May 7, six weeks early.
Although the hospital’s nurses and social workers tried their best to connect Ms. Mayer with her son, sharing daily pictures and placing a phone in his basinet so they could “talk,” the physical separation left her fearing she and Isaac wouldn’t bond.
“He doesn’t know me,” Ms. Mayer said in a phone interview after she, but not Isaac, had been discharged from the hospital. “I know I carried him for 34 weeks, but he doesn’t know who I am. I’ve only held him once. He’s 12 days old.”
Like Ms. Worek, Ms. Mayer was not vaccinated. She, too, was a touch nervous about the shot and had come to see the virus as not much of a threat. She was on leave from her job as a homecare personal support worker when she got sick. She doesn’t know how the virus found its way into the home she shares with her fiancé and three of her children.
“It’s going to sound bad,” Ms. Mayer said, “but I was working in the field every day and working with people that were COVID positive. And I didn’t catch it. I was like, ‘Oh, maybe it’s not as bad as people are making it seem,’ which was very wrong of me to think.”
She and Ms. Worek are now urging other pregnant women to get vaccinated right away.
“What if I would have got the vaccine and then I got COVID and I didn’t get as sick?” Ms. Mayer said. “The baby would still be inside of me.”
More: Women on the front lines
In April, The Globe and Mail caught up with emergency-room doctor Kanna Vela at her old high school, where she was helping with the Scarborough Health Network’s pop-up vaccine clinic.
The Globe and Mail
Our Morning Update and Evening Update newsletters are written by Globe editors, giving you a concise summary of the day’s most important headlines. Sign up today.
 Kelly Grant
Kelly Grant