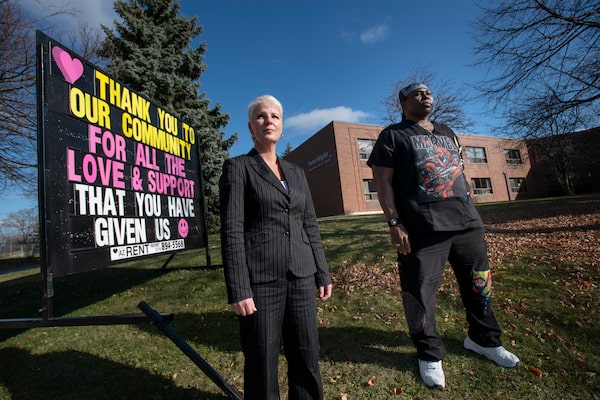
Julie Streit, left, recreational director at Forest Heights Long Term Care, and her partner Emmanuel Sambi, a personal support worker at the home, are seen here on Nov. 14, 2020.Fred Lum/The Globe and Mail
When the first resident of Forest Heights died of COVID-19 on April 9th, Julie Streit was at his bedside, saying a prayer. The next day, another resident was struggling to breathe. Then another. Ms. Streit, the recreation manager and palliative care team lead for the long-term care home in Kitchener, Ont., raced between rooms, offering comfort as best she could, hoping each case would be the last. Instead, death came faster.
In the frenzy of cleaning and feeding and medical care, her job was to make a quiet space for compassion. When a resident’s eyes showed fear, she would pull down her mask so they could see her smile, or remove a glove to touch them. It was against the rules. “But I didn’t want them to feel a plastic hand,” she says. Not when so much that was human had already been stolen away.

Forest Heights Long Term Care home in Kitchener, Ont. on Nov. 11, 2020.Fred Lum/The Globe and Mail
“No one should die alone,” she says, “not unless it is their choice.”
Ms. Streit watched COVID-19 take 49 lives – a crushing number that must surely make her one of this country’s most expert witnesses to the pandemic’s terrible price.
For all but a handful of cases, family members were too far away to come, too vulnerable to the virus themselves, or too scared. Ms. Streit would call when death was close, and hold the phone for last goodbyes. When a family put “I love you” signs on the fence outside, she didn’t tell them that Papa was no longer awake to see them, that the best she could do was whisper a description in his ear. She would talk sons and daughters out of face-timing at the very end so they wouldn’t have the image of their mom gasping for breath. She could protect their memories, at least. As for herself, she says, “No one can help me un-see what I have seen.”
“We are broken. We are sad,” Ms. Streit wrote in a letter read at the Ontario inquiry into how long-term care homes handled the pandemic. Struggling to describe this past spring, she called it “hell, a bad nightmare, a war with no winners.” There was, she wrote, “no time to cry; no time to say goodbye; no time to rest.”
No time to do death properly. In the early days after the virus found its way inside, 15 of her 19-member palliative team tested positive themselves, including the chaplain. Ms. Streit was the one the overworked nurses and personal support workers would call to the room when death was near, again and again. She knew who had distant grandchildren to call, who hoped to mend family fences before the end, and who had no one.
For one dying resident, an Elvis fan, she stumbled through the words of Can’t Help Falling In Love as best she could remember. “I knew I was fumbling them,” she says. But it didn’t matter. Cast into darkness, a memory lands. “You just saw his face relax.”

Julie Streit, the Recreation Director, is photographed outside Forest Heights Long Term Care, on Nov 14 2020.Fred Lum/The Globe and Mail
When her legs ached from squatting so long at the bedside of one resident – his goodbyes all said, ravaged by cancer and the virus – she sat on the floor, weeping and wondering what more she could do, how to keep going. Other residents needed her, anxious families sought her counsel, the work phone never stopped ringing. “Maybe I was tired, maybe I was just a bit broken,” she says, “but I just wanted him to go.” Then she wouldn’t feel guilty about leaving him alone, one more ache to carry. Sometimes when she prayed, “I was praying for myself, too.”
One night, she went home at the end of a 16-hour shift, after trying to persuade a favourite resident to go to the hospital after he tested positive. “You can’t make me,” he said, in his usual bantering way, and she thought, “I will try again tomorrow.” He was in his 50s and physically fit, which improved his odds. But in the morning, he was gone. That’s how it went. The 90-year-old whose choking breaths could be heard in the hallway for days is still alive. The quirky resident, still years from senior status, who used the stationary bike every day, is not. His was one of only two deaths that she wasn’t present for. “I would have had a different conversation,” she says, her voice breaking. “I thought there was time.”
Before the pandemic, the funeral directors would come after the family had paid respects, and do their work. There would be a “dignity walk” to the front door, with an honour guard of residents lined along the path, a celebration of life in the moment of death.

Forest Heights Long Term Care home in Kitchener, Ont. Nov 11 2020.Fred Lum/The Globe and Mail
None of that could happen. For the first time in her long career, Ms. Streit helped prepare the bodies, so they could be removed quickly, and not risk spreading the virus. Working together, two staff would zip the body into a white bag, write “COVID Positive” across it with a Sharpie, and bring the gurney down in an empty elevator. They took turns because this was the task that really broke people. In the beginning, those bodies would go out the back door, but Ms. Streit put a stop to that. “Garbage goes out the back door,” she says. “Residents go out the front door, the way they entered.”
In her letter, Ms. Streit wrote, “I do not feel.” It is not true, as she well knows. The feelings are there, pushed deep by the distraction of needing to work, to be dealt with later. Even now, the virus still knocks at the door, kept at bay by protocols, and luck. Whatever the winter brings, there will be hands that need holding, and songs to sing.
Sign up for the Coronavirus Update newsletter to read the day’s essential coronavirus news, features and explainers written by Globe reporters.
 Erin Anderssen
Erin Anderssen