
Illustration by The Globe and Mail
As a global pandemic began to take root in February, China held a series of backchannel conversations with Canada, lobbying the federal government to keep its borders open.
With the virus already taking a deadly toll in Asia, Heng Xiaojun, the Minister Counsellor for the Chinese embassy, requested a call with senior Transport Canada officials. Over the course of the conversation, the Chinese representatives communicated Beijing’s desire that flights between the two countries not be stopped because it was unnecessary.
“The Chinese position on the continuation of flights was reiterated,” say official notes taken from the call. “Mr. Heng conveyed that China is taking comprehensive measures to combat the coronavirus.”
Canadian officials seemed to agree, since no steps were taken to restrict or prohibit travel. To the federal government, China appeared to have the situation under control and the risk to Canada was low. Before ending the call, Mr. Heng thanked Ottawa for its “science and fact-based approach.”
Around the same time, with the death toll rising and the virus spreading internationally, preparations were made for a phone call between Minister of Foreign Affairs François-Philippe Champagne and his Chinese counterpart. According to speaking notes prepared in advance of that discussion, Canada’s key messages were to “express sympathy” and to convey how “impressed” Ottawa was with “efforts deployed to contain the outbreak, and the transparent approach taken by China thus far.”
The government had “full confidence” in China’s ability to contain the virus.
It was a critical moment in the looming pandemic, but the Canadian government lacked the full picture, instead relying heavily on what Beijing was choosing to disclose to the World Health Organization (WHO). Ottawa’s ability to independently know what was going on in China – on the ground and inside hospitals – had been greatly diminished in recent years.
Canada once operated a robust pandemic early warning system and employed a public-health doctor based in China who could report back on emerging problems. But it had largely abandoned those international strategies over the past five years, and was no longer as plugged-in.
By late February, Ottawa seemed to be taking the official reports from China at their word, stating often in its own internal risk assessments that the threat to Canada remained low. But inside the Public Health Agency of Canada (PHAC), rank-and-file doctors and epidemiologists were growing increasingly alarmed at how the department and the government were responding.
“The team was outraged,” one public-health scientist told a colleague in early April, in an internal e-mail obtained by The Globe and Mail, criticizing the lack of urgency shown by Canada’s response during January, February and early March. “We knew this was going to be around for a long time, and it’s serious.”

Wuhan, the epicentre of China's COVID-19 outbreak, as shown on Feb. 13 during lockdown, and on Dec. 7, when restrictions were mostly lifted.Getty Images
China had locked down cities and restricted travel within its borders. Staff inside the Public Health Agency believed Beijing wasn’t disclosing the whole truth about the danger of the virus and how easily it was transmitted. “The agency was just too slow to respond,” the scientist said. “A sane person would know China was lying.”
It would later be revealed that China’s infection and mortality rates were played down in official records, along with key details about how the virus was spreading.
But the Public Health Agency, which was created after the 2003 SARS crisis to bolster the country against emerging disease threats, had been stripped of much of its capacity to gather outbreak intelligence and provide advance warning by the time the pandemic hit.
The Global Public Health Intelligence Network, an early warning system known as GPHIN that was once considered a cornerstone of Canada’s preparedness strategy, had been scaled back over the past several years, with resources shifted into projects that didn’t involve outbreak surveillance.
However, a series of documents obtained by The Globe during the past four months, from inside the department and through numerous Access to Information requests, show the problems that weakened Canada’s pandemic readiness run deeper than originally thought. Pleas from the international health community for Canada to take outbreak detection and surveillance much more seriously were ignored by mid-level managers inside the department. A new federal pandemic preparedness plan – key to gauging the country’s readiness for an emergency – was never fully tested. And on the global stage, the agency stopped sending experts to international meetings on pandemic preparedness, instead choosing senior civil servants with little or no public-health background to represent Canada at high-level talks, The Globe found.
An internal study obtained by The Globe suggests people inside the department were aware of some of these issues. Meanwhile, documents and interviews with current and former employees who have come forward in recent months indicate the mishandling of the pandemic early warning system was a symptom of broader problems affecting the agency. A cascade of decisions over the past decade, each critically important in their own right, left Canada struggling to effectively process what was happening in China in real time early this year, which hampered its ability to respond quickly.

A man gets tested for COVID-19 at a pop-up clinic in Scarborough this past May.Nathan Denette/The Canadian Press
The curtailing of GPHIN and allegations that scientists had become marginalized within the Public Health Agency, detailed in a Globe investigation this past July, are now the subject of two federal probes – an examination by the Auditor-General of Canada and an independent federal review, ordered by the Minister of Health.
Those processes will undoubtedly reshape GPHIN and may well lead to an overhaul of how the agency functions in some areas. The first steps will be identifying and fixing what went wrong. With the country now topping 535,000 cases of COVID-19 and more than 14,700 dead, there will be lessons learned from the pandemic.
Prime Minister Justin Trudeau has said he is unsure what role added intelligence could have played in the government’s pandemic response, though he regrets not bolstering Canada’s critical supplies of personal protective equipment sooner. But providing the intelligence to make those decisions early is exactly what GPHIN was created to do – and did in previous outbreaks.
Epidemiologists have described in detail to The Globe how vital it is to move quickly and decisively in a pandemic. Acting sooner, even by a few days or weeks in the early going, and throughout, can have an exponential impact on an outbreak, including deaths. Countries such as South Korea, Australia and New Zealand, which have fared much better than Canada, appear to have acted faster in key tactical areas, some using early warning information they gathered. As Canada prepares itself in the wake of COVID-19 for the next major health threat, building back a better system becomes paramount.
Experts in intelligence gathering and warning detection say there’s no way for the government to know what information it did not have. And there is a price to pay for that. “Doing intelligence by shutting off your right ear is guaranteed to fail,” said Lieutenant-Colonel Paul O’Leary, who is now retired but spent 40 years in Canada’s military and intelligence community.
Favouring certain channels of information and disregarding others is risky, he said. “You’re headed for failure – unless you get awful lucky.”

Family members visit their mother at an Abbotsford, B.C. care home. Using limited information, the federal government repeatedly said the virus posed a low risk to Canada.Darryl Dyck/The Canadian Press
‘I CANNOT UNDERSTAND’
Concerns about Canada’s readiness for a pandemic weren’t limited to scientists inside the Public Health Agency.
Internal documents and e-mail correspondence obtained by The Globe show senior officials at the WHO had also been growing increasingly frustrated in recent years with the direction Ottawa was taking.
This included the government’s oversight of GPHIN, which the WHO had praised as a “foundation” of global outbreak response.
Created in the 1990s, GPHIN was a sort of smoke detector for international health threats, sorting through open-source data from around the world looking for signs of trouble, processing it using the knowledge of epidemiologists, then alerting the international community.
Described by the government as a “24/7 curated situational awareness service,” it operated like a detective agency for outbreaks, with a small team of highly specialized analysts working in multiple languages, scouring millions of news and health data points around the world, listening for hints of a possible outbreak.
But years of restructuring weighed heavily on the Public Health Agency over all. A wave of budget cuts that began under the Stephen Harper government in 2012, followed by a series of key personnel changes, began to reshape how the department operated.
In an effort to restructure how Public Health ran, the agency saw an influx of senior civil servants from around the government, brought in to fill management roles despite having very little or no training in public health. Soon, there was an exodus of scientific expertise, according to more than a dozen current and former staff members who spoke to The Globe, including scientists, senior advisers and directors.
In 2018, senior managers set their sights on reconfiguring GPHIN. Under Jim Harris, director-general of the Centre for Emergency Preparedness and Response at the time, and Sally Thornton, vice-president of the Health Security Infrastructure Branch, the pandemic early warning system was seen as too internationally focused. Management believed parts of GPHIN’s $2.8-million annual budget could be better spent on domestic projects, so its operations were curtailed.
The changes alarmed the WHO.
Senior officials at the Geneva-based organization – including Philippe Barboza, a manager of the WHO’s Health Emergencies Programme – urged Canada not to let its home-grown pandemic warning system falter. The highly specialized unit wasn’t merely a benefit to Canada – it had grown to fill a critical international role, providing the WHO with one-fifth of its epidemiological intelligence. It was too important to be curtailed.
But those efforts failed. There had been numerous turnovers among senior management at Public Health over the years, and the people who understood the intrinsic value of the early warning system were no longer in charge.
On Nov. 2, 2018, Abla Mawudeku, an epidemiologist who helped build GPHIN into a system respected around the world, wrote an e-mail to a group of colleagues in the international pandemic surveillance community, informing them that the WHO’s bid to change Ottawa’s mind had fallen short.
“I would like to let you know that, sadly, we have not been successful in convincing management of the critical value and role of GPHIN within and outside of Canada, and the indispensable relationship with the WHO,” Ms. Mawudeku wrote in e-mails that were obtained by The Globe from a third-party source. “It is clear that today’s leadership is charting a different path that does not incorporate the long-term vision of GPHIN, and could lead to the demise of the GPHIN program.”
It was the moment Canada let its world-renowned pandemic early warning system slip.
“GPHIN has survived many obstacles, but this challenge appears to be insurmountable at this time,” Ms. Mawudeku concluded.

The World Health Organization's headquarters in Geneva.Anja Niedringhaus/The Canadian Press
The move stunned epidemiologists at the WHO. In e-mails obtained by The Globe, Dr. Barboza confided with colleagues that he was left speechless by the Canadian government’s decision, which not only affected Canada but much of the world, as well. Though others were attempting to create similar systems around the world, including government programs and for-profit enterprises, they weren’t nearly as robust.
“Although I know too well how much politicians can be short-sighted, I still can’t understand how people in Canada cannot see the value in GPHIN for domestic issues and for the world,” Dr. Barboza wrote in an e-mail to Public Health epidemiologists in Canada. “GPHIN has been a pioneer in what was, at that time, a totally barren field. I cannot understand that this is not recognized.”
Dr. Barboza did his best to end on a hopeful note. “We have to find other alternatives to push forward,” he said. “The war is not lost yet. I’m sure we will find something.”
But he was wrong.
Over the next year, a key part of the GPHIN system fell silent. A department edict from Mr. Harris and Ms. Thornton ordered GPHIN’s analysts to cease issuing outbreak warnings without first obtaining senior management approval. Soon the alerts stopped, and detection efforts were curtailed.
Analysts were reassigned to other work that did not involve outbreak surveillance, and staffing hours were cut. Soon, GPHIN was no longer the 24/7 operation the government purported it to be.
Requests to interview Mr. Harris, who has since transferred to another department, and Ms. Thornton, who left in September, have been declined by the government.
As a Globe investigation revealed in July, GPHIN ceased issuing international alerts on May 24, 2019, less than eight months before the outbreak in China became known to the world.
Although some GPHIN information was still used internally at PHAC after the outbreak began, the unit was a shadow of its former self.
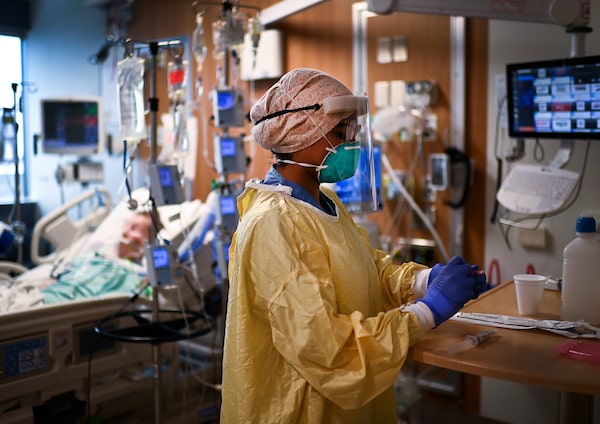
A COVID-19 patient at Toronto’s Humber River Hospital. Concerns about Canada’s pandemic readiness weren’t limited to scientists at Public Health.Nathan Denette/The Canadian Press
GROWING TENSIONS AND GOVERNMENT PERKS
The GPHIN problem was a symptom of a bigger ailment inside the Public Health Agency – one where expertise took a back seat to policy, and scientists increasingly found themselves marginalized.
According to internal documents provided to The Globe in recent months, by the time the pandemic early warning system was curtailed last year, the Public Health Agency was already struggling with these concerns. The restructuring that began under the Harper government, bolstering management with senior civil servants who lacked training in public health, remained mostly unchanged under Trudeau, and the problems went unchecked.
Doctors and epidemiologists said they found themselves outranked by bureaucrats who held organizational clout over important decisions, including department priorities, strategy and budgeting. This led to tension, particularly as senior government officials began to replace public-health experts in key roles, including on international panels.
Such panels involve trips to Europe, Asia and elsewhere – perks that came to be seen within the agency as the domain of senior civil servants, rather than rank-and-file experts.
Department records illustrate one example of this trend. In September, 2018, a Canadian specialist on outbreak surveillance systems was invited by the WHO to attend a high-level gathering of pandemic preparedness experts in Geneva. The summit, whose purpose was “to advance our collective efforts for the early detection, verification and assessment of health risks,” was to be held over three days, with costs covered by the WHO.
In its invitation, the WHO went so far as to detail the type of people it wanted at the discussion. Specifically, it needed first-hand expertise. “This is a technical meeting and workshop. We therefore invite [governments] to send appropriate representatives in order to ensure the objectives are met,” the WHO said. “Participants must be able to actively contribute to the conversations on requirements, options and solution development – and should therefore be routinely engaged in public health intelligence and event-based surveillance activities.”
But when the department decided who would represent Canada at the summit, it chose not to send the specialist who worked closely with GPHIN. Instead, a more senior bureaucrat went to Switzerland.
The decision upset epidemiologists and other staff inside the department for the signal it sent – that managerial seniority carried more clout than expertise.
Elizabeth Gooding, a director within the department’s Centre for Emergency Preparedness and Response, instructed the specialist to provide the higher-ranking colleague with whatever technical information was required to represent Canada at the summit.
“There is no way to convey years of experience,” the person told Ms. Gooding in an e-mail obtained by The Globe. “It would take too long, and her competencies rest elsewhere.”
In response, Ms. Gooding reminded the surveillance expert that “briefing up” – providing information for the more senior colleague to present on their behalf – “is actually a really nice way to interact as a team!”
When the WHO learned of this decision, Philip Abdelmalik, an epidemiologist who leads the organization’s Detection, Verification and Risk Assessment Unit, could not understand Canada’s logic. “I’m not reserving my words; I just don’t have any. Stunned,” Dr. Abdelmalik told a group of Canadian epidemiologists in an e-mail.
Dr. Abdelmalik had his own experience with such problems at the agency. Having left Ottawa to work at the WHO, he was an example of the brain drain of public-health experts who departed in frustration, fearing the focus inside the department had begun to shift away from science.
One of the breaking points for Dr. Abdelmalik was a failed attempt by Public Health and the National Research Council to upgrade GPHIN in order to expand Canada’s pandemic preparedness capacity. In a document Dr. Abdelmalik submitted to Public Health management in late 2017, titled “Exit Report,” which was obtained by The Globe, he described “growing tensions” inside the government over GPHIN, and questioned the “competency and understanding” of those overseeing the upgrade, since they lacked experience with the pandemic early warning system.
But the watering down of scientific capacity inside Public Health had been going on for some time.

David Butler-Jones, shown in 2009, was Canada's first Chief Public Health Officer.Sean Kilpatrick/The Canadian Press
Early this year, Dr. David Butler-Jones, Canada’s first Chief Public Health Officer (CPHO), warned about the erosion of expertise and its impact. Canada, he said, has “replaced public-health managers and analysts with generic public servants. Resources, expertise and capacity have been reduced, and expertise positioned further away from where organizational decisions are made on budget, policy, communications, programs and services, and so forth.”
This has had an impact on how the department prepares for a crisis in the years between outbreaks. “There is good reason that medical specialists in public health and preventive medicine require five-plus years of postgraduate training after medical school,” he said. “To understand and apply public health effectively requires expertise in everything from epidemiology and statistics, to prevention and control of disease and injury, to health policy.”
Michael Garner, a former senior science adviser who spent 13 years at the agency before leaving last year, said the influx of senior bureaucrats who lacked an understanding of public health resulted in science being “sidelined” and slowed the department’s ability to handle urgent problems effectively. “Scientists and public health professionals at PHAC have not had their opinions and expertise valued. As a result, decisions impacting the health of the public that PHAC makes are not adequately rooted in scientific knowledge and public-health science,” Mr. Garner said in an interview.
Both he and Dr. Butler-Jones argue the installation of a president at the top of the agency – a role introduced by the Harper government and kept in place under Mr. Trudeau – changed the overall direction of the department. The move tilted the balance of power, relegating the CPHO (a title now held by Dr. Theresa Tam) to the role of adviser and spokesperson, which filtered down through the management ranks that handle day-to-day operations.
“The decision to place a generic bureaucrat rather than a public-health scientist at the top of the Public Health Agency has created a cascade where public-health experts are no longer present at the senior levels of the agency,” Mr. Garner said.
The trend became worrisome enough that some scientists suggested the department create an internal crash course in public health so that new additions to the agency could learn the basics on the fly. But it was never adopted.
Among the most important international groups Canada belongs to, from a pandemic preparedness standpoint, is the Global Outbreak Alert and Response Network, or GOARN. It was created 20 years ago as a network of public-health agencies, laboratories and institutions that could mobilize resources in response to emerging epidemics in support of the WHO, including deploying containment experts and investigators to the centre of an outbreak.
“GOARN has investigated hundreds of epidemics and outbreaks in various countries,” said Canadian epidemiologist Ronald St. John, who created Canada’s pandemic early warning system in the 1990s and headed the agency’s Centre for Emergency Preparedness and Response. He also served as GOARN’s first chairman.
“It is an effective tool,” Dr. St. John said. “But it’s technical. I mean, it’s medical and it’s technical.”
But in recent years, the agency stopped sending public-health experts to represent Canada on the committee, which is based in Geneva. Canada’s representative at GOARN meetings is Ms. Gooding, a department director.
Until recently, Ms. Gooding was listed on the GOARN website as a doctor. However, a check of her credentials shows Ms. Gooding has a master’s in business administration from Carleton University in Ottawa.
In fact, Canada is the only member on the 21-person GOARN steering committee whose representative has no formal grounding in medicine or public health. The others are predominantly epidemiologists and doctors who specialize in rare viruses, infection control or outbreak surveillance.
On Oct. 30, The Globe submitted a list of questions to the Public Health Agency. The questions included why Canada is an outlier on the committee; why the agency doesn’t send a subject-matter expert to serve on a high-level group such as GOARN; and why Ms. Gooding is listed on the website as a doctor when she is not. Neither the department nor Ms. Gooding responded, despite several reassurances from a government spokesperson that answers would be provided.
However, in early November – roughly a week after the questions were submitted by The Globe – her curriculum vitae on the GOARN website was updated.
She is no longer listed as a doctor.

Theresa Tam commissioned a report in late 2018 that sought to evaluate the department. Finished in late 2019, it warned Public Health may lack the expertise and experience needed in a crisis.Sean Kilpatrick/The Canadian Press
NOT PREPARED
Some staff inside Public Health say they grew concerned about the agency’s work on pandemic readiness in recent years. The message circulating inside the department was straightforward: “We are not prepared” for a major outbreak.
The government’s records indicate those concerns were not unfounded. Though Public Health was in the early stages of evaluating its most recent pandemic response plan, formulated in 2017, it never got around to fully testing it.
A department spokesman said the Centre for Emergency Preparedness and Response held a workshop on a draft version of the plan in 2017, followed by a meeting known as a table-top discussion in 2018. But an epidemiologist with direct knowledge of the process described those as preliminary steps – mostly paper analysis and boardroom discussions – not an actual drill to practice the government’s overall response to an outbreak, or identify weaknesses that need to be fixed.
A full-scale exercise to test Canada’s pandemic preparedness plan was scheduled for this year, staff said, but was cancelled. An actual pandemic had struck first.
Several of the problems afflicting the Public Health Agency were known within the department.
The Globe obtained an internal government report completed last year, in which PHAC staff worried Canada was ill-prepared for a pandemic, in part because the department lacked funding, direction and scientific experience.
The research paper, which was obtained through Access to Information, was commissioned in late 2018 by top management at the agency, including Chief Public Health Officer Dr. Tam, to determine how the department was perceived, its strengths and weaknesses, and what needed to be done in the years ahead.
Just over a year into her term, Dr. Tam had essentially commissioned a review of her own department – or at least the beginnings of one.
Between March and July, 2019, two respected Canadian public-health doctors, Perry Kendall and Richard Massé, interviewed 49 people, including managers, public-health experts and analysts inside the department, as well as some in the international medical community.
The answers the report came back with were blunt and unsettling. The interview subjects, who were granted anonymity by Dr. Kendall and Dr. Massé, described a department stretched thin by a sprawling mandate, sparse funding and a deteriorating culture. Canada was “under-prepared for major events such as a devastating pandemic,” one subject warned. “For such events, we have little comparable experience, gaps in mandates, and little mobilization capacity or field knowledge.”
Several interviewees said the Public Health Agency began to deteriorate between 2012 and 2015, an era they refer to as a “dark period” of budget cuts and personnel changes that altered its culture.
Initially staffed by doctors and epidemiologists, the government believed Public Health needed stronger management from other departments. But according to the report, that created unintended consequences.
“The initial decision to staff senior management with mostly physicians, while sound from a public health perspective, resulted in an agency that seemed poorly integrated into ‘official Ottawa’ and weakly managed,” the report said. “This, followed by a counter-move – the recruitment of more professional civil servants – brought better administrative know-how, but less understanding of the core competencies of public health.”
The result was a department that lacked critical scientific knowledge in key jobs. “Many interviewees felt that the agency was still under-resourced for its mandate, with frequent changes of people,” the report said. “Even in priority areas, very junior people without much experience were appointed with subsequent loss of [expertise] but added bureaucracy.”
The report zeroed in on the creation of the president role as a problem, since it effectively reduced the CPHO to an adviser, which some people saw as “an effective demotion,” while the president was politically appointed.
This took direct oversight of programs and budgets away from the CPHO, whose job was to plan for a pandemic even when threats seemed remote, and ultimately hurt the agency’s ability to do the job it was created for, the interview subjects told Dr. Kendall and Dr. Massé.
“Many had hoped for an agency with an independent voice speaking and advocating for the health of Canadians, not embedded in the political system,” the report said. “For many interviewees that vision was never fully realized. The agency is seen as more closely resembling a regular government department with the accompanying bureaucracy and inertia.”
The paper called for the government to rebuild PHAC with more focus on science – and warned, ominously, that Public Health may lack the “expertise, trust and experience” needed in a crisis.
The 39-page report, titled “Preparing PHAC for the Future,” was submitted to the government on Oct. 8, 2019.
In less than three months, the COVID-19 outbreak would have the world on its heels.
SOMETHING HAPPENED BETWEEN THEN AND NOW
David Heymann remembers the pandemic response system Canada once pioneered globally and wonders where it went.
A renowned epidemiologist who helped identify and contain the first Ebola outbreak in 1976, Dr. Heymann spent 22 years at the WHO and was its executive director for communicable diseases in the late 1990s. That’s when he first learned of GPHIN and what Canada was building.
“This was quite a powerful tool,” said Dr. Heymann, who is now a professor at the London School of Hygiene and Tropical Medicine.
“All of a sudden, we [at the WHO] were getting much more information from GPHIN than we were getting from member countries.”
He knew all too well that governments often played down or denied outbreaks to protect their own reputation or economic interests. But by analyzing streams of medical data and snippets of news reports from around the world, Canada’s early warning system could often find the faintest signals of a looming problem and get that information to the right people.
“One time I was speaking with a Minister of Health in Africa who wouldn’t report an Ebola outbreak,” Dr. Heymann recalled. “And I said, ‘Well, I found this out [from GPHIN], and if you don’t report it and your neighbouring countries get infected, they are going to be very unhappy with you.’ That forced him to report it officially and invite the WHO to help the country. So GPHIN was very useful.”
It changed how countries thought and what they could get away with. Sometimes the warnings came early enough to contain an outbreak and mitigate the damage.
“When countries realized that we were getting information [at the WHO] that could embarrass them because they didn’t report it,” Dr. Heymann said, “they began reporting in a much better way than they had before.”

David Heymann, shown in 2016, said GPHIN revolutionized how outbreaks could be detected.FABRICE COFFRINI/AFP via Getty Images
Although it’s impossible to know after the fact what impact a fully functioning GPHIN would have had on Canada’s response to the COVID-19 outbreak, people familiar with outbreak detection suspect the earliest signals of COVID-19 could have been evident in China weeks, or even months, before the world learned of the crisis. GPHIN can’t know what it didn’t find, because it wasn’t watching as closely as it once did.
Even after the virus became widely known, better use of intelligence in January and February, when China was still playing down the outbreak, could have injected urgency into Canada’s response.
One of the key lessons Canada learned from the 2003 SARS crisis was that more intelligence was needed for pandemic threats. China’s actions this year – from muzzling its own doctors and erasing criticism from the internet, to arresting journalists who tried to report on the COVID-19 outbreak – shows how hard it can be to come by reliable information in times of emergency.
It was the same in 2003. Although the SARS outbreak turned deadly in Canada, killing 44 people, the data gathered early on by GPHIN and shared internationally during that crisis revealed hidden clues about the severity of the outbreak in China, Dr. Heymann said. That likely helped lessen the blow.
“It was extremely important, because China was not forthcoming,” he said.
As the government launches its independent review into the oversight of the pandemic early warning system and the problems faced by scientists inside the Public Health Agency, Dr. Heymann hopes GPHIN emerges from the process stronger and that the world embraces similar systems.
“The investment that Canada made back in the 1990s revolutionized the way clusters of disease and outbreaks could be detected,” Dr. Heymann said. “It was a change that brought us really into the 21st century as far as disease detection goes. And I think the Canadian government should really be lauded for that.”
But, he added, “something happened between then and December, 2019.”
In depth: Canada and vaccinations
Science reporter Ivan Semeniuk outlines how Canada benefited from researchers working in parallel and accelerated the approval process to have safe COVID-19 vaccines ready so quickly.
Sign up for the Coronavirus Update newsletter to read the day’s essential coronavirus news, features and explainers written by Globe reporters and editors.
 Grant Robertson
Grant Robertson