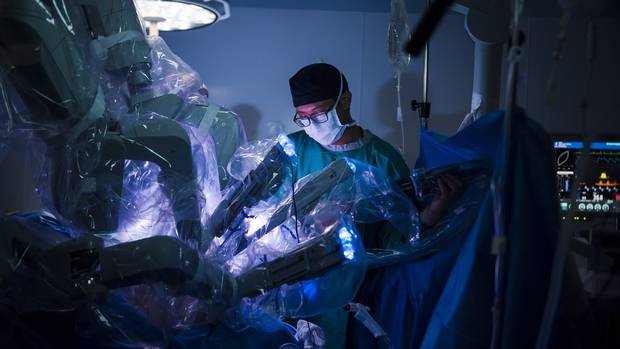
The patient, a 70-year-old man with high-risk prostate cancer, was a Jehovah's Witness.
His religion was one of the reasons he decided to undergo surgery at St. Joseph's Healthcare in Hamilton, home to a robot named da Vinci whose steady metal hands can remove a prostate with scant risk of the blood transfusions forbidden by the man's faith.
On a recent afternoon, the patient laid unconscious on an operating table as surgeon Bobby Shayegan and his team plunged a camera and three robotically controlled surgical instruments through small incisions in his abdomen.
Dr. Shayegan settled himself in front of a three-dimensional screen, clasped the two joysticks that controlled the tools inside his patient's pelvis and proceeded to cut, cauterize and stitch until he freed the man's prostate, pulling it out through one of the original incisions.
There was next to no blood.
"That was routine," Dr. Shayegan said afterward, holding the plum-sized gland that he and the robot had removed together. "Very routine."
This is how nine out of 10 prostatectomies are carried out in the United States. Robot-assisted surgery isn't the way of the future there – it's the way of now.
But in Canada, where robotic operations are much less common, a new recommendation against public funding for robot-assisted prostatectomies has physician leaders warning this country could fall even further behind the rest of the developed world when it comes to offering cutting-edge medical procedures.
In its first real ruling on a robotic surgery, the expert committee that advises Ontario on which new health technologies to pay for said there was no good evidence that robot-assisted radical prostatectomy is any better than conventional open surgery when it comes to controlling cancer or preserving urinary and sexual function.
The panel said the robot's other benefits – patients have smaller incisions, lose less blood, suffer less pain and leave the hospital sooner – were not significant enough to justify spending, on average, an extra $3,224 a case, a figure that does not include the millions that wealthy benefactors have spent buying the machines for Canadian hospitals.
"We don't have unlimited resources," said Irfan Dhalla, vice-president of evidence development and standards at Health Quality Ontario, the agency that oversees the Ontario Health Technology Advisory Committee, known as OHTAC. "How do we spend the resources we do have to maximally benefit the people of Ontario?"
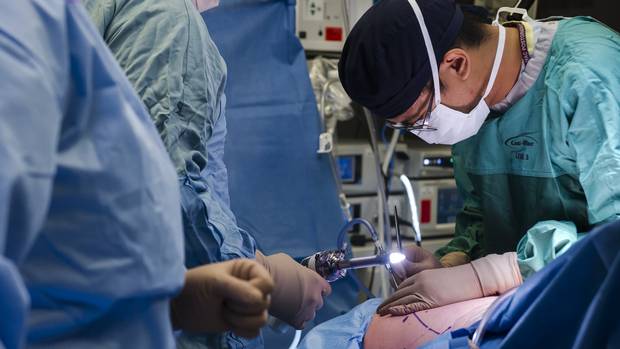
Incisions are made for the ports through which robotic arms work within the body of the patient. This is how nine out of 10 prostatectomies are carried out in the United States.
Chrstopher Katsarov/the Globe and Mail
OHTAC's recommendation, which is in the hands of Ontario's health ministry, has sparked an outcry.
Four urologists and one general surgeon who advised OHTAC during its research asked that their names be removed from the final recommendation paper, published last month, because they disagreed so strongly with its conclusions. Urologists and chiefs of surgery at major teaching hospitals wrote letters, begging the committee to reconsider.
"This is a harbinger of bad things to come," said James Rutka, chair of the surgical division at the University of Toronto's medical school.
The fight over public funding for robot-assisted prostate surgery in Canada's most populous province could have ripple effects in other provinces, and on other types of robotic surgery for which the benefits are more clear cut.
It could also sour top-flight surgical trainees on Canada, Dr. Rutka warned.
More profoundly, the fight raises a question: Should a public health-care system with little money to spare pay for a costly new technology when the old-fashioned approach might work just as well?
When doctors talk about robotic surgery, they're usually talking about the da Vinci Surgical System.
Named for the renaissance genius and manufactured by a California company called Intuitive Surgical Inc., the da Vinci is the only full-scope surgical robot licensed by Health Canada. (The regulator has approved two other robotic technologies with some limited surgical capabilities, but none that can do what the da Vinci can.)
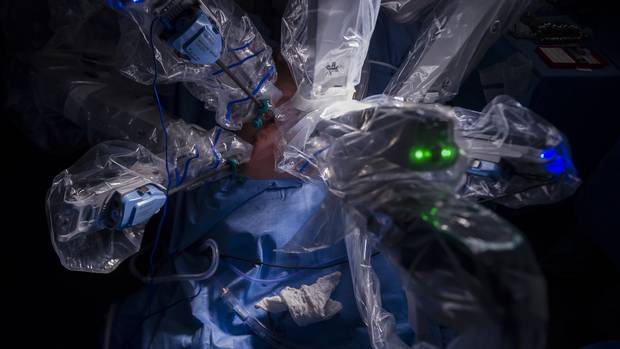
Robotic arms are seen protruding from a patient’s abdomen, allowing for fine surgical maneuvers. Robotic prostatectomy is performed at St. Joseph’s hospital in Hamilton on Thursday, July 27, 2017.
Christopher Katsarov/the Globe and Mail
Describing the machine as a robot can be a little misleading. It does not look like Johnny 5 from Short Circuit, or operate on autopilot as robotic technology does in other fields.
Rather, the da Vinci is a tall podium with four robotic arms, each outfitted with a different tool whose every movement is controlled remotely by a surgeon.
The arms have "wrists" that are more supple than a human wrist, allowing surgeons to do things they couldn't with their own hands.
The first da Vinci model was approved by the U.S. Food and Drug Administration (FDA) in 2000. The machines spread rapidly across the U.S. health-care landscape, fanned by patient and surgeon demand and aggressive marketing.
"They had these robots rolled out at half-time events and state fairs and malls," said Martin Makary, a professor of surgery at the Johns Hopkins University School of Medicine in Baltimore who researched the reporting of complications in surgical robots. "The public was dazzled by this thing."
Today, more than 4,100 da Vinci surgical systems are installed around the world, 2,703 of them in the United States, and 31 in Canada, according to Intuitive.
Urology was the first specialty to welcome its new robot overlords.
Part of the reason is that removing the prostate laparoscopically – a less sophisticated key-hole technique used commonly in other operations – is so difficult that relatively few surgeons have mastered it.
The male pelvis is a narrow work site packed with trip wires. Nick the bladder or rectum, and a patient winds up incontinent.
The prostate itself is located between the bladder and the penis; after surgeons remove the gland, they have to stitch together the bladder and urethra with enough precision to create a watertight seal.
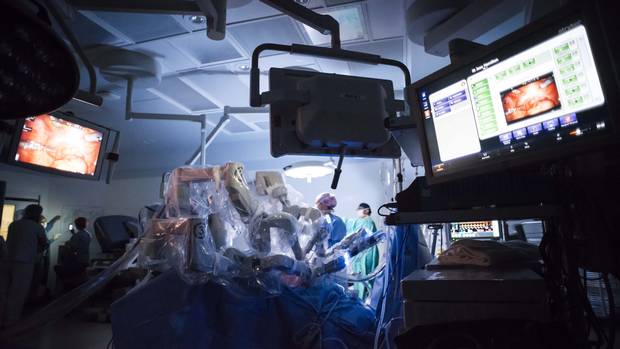
Dr. Bobby Shayegan operates in the background through a monitor. Using a robot to perform a prostatectomy means the procedure is far less invasive.
Christopher Katsarov/the Globe and Mail
"There's not a lot of room for error," said Dr. Shayegan, who is also the clinical director of the Boris Family Centre for Robotic Surgery in Hamilton.
The da Vinci system made it possible for more urologic surgeons to confidently offer their patients a minimally invasive prostatectomy.
Now, about 90 per cent of radical prostatectomies in the United States are performed robotically. The number isn't as high in Britain (50 per cent) or Australia (58 per cent), but it's much higher than in Canada, where about 30 per cent of prostatectomies are done with the help of a robot, according to the OHTAC report.
But in the rush to adopt the da Vinci technology, few researchers conducted randomized controlled trials comparing robot-assisted prostatectomy to open surgery, the gold standard in evidence.
"One of the stories here," Dr. Dhalla said, "is why isn't there good evidence?"
He estimated that hundreds of thousands of men around the world have had a robot-assisted prostatectomy, "and there's been one, tiny randomized control trial in Australia with about 300 patients comparing the open approach with the robotic approach."
That Australian study, published a year ago in The Lancet, was the foundation of OHTAC's thumbs-down for robot-assisted prostatectomies.
The study, which followed 157 men who underwent robot-assisted surgery and 151 who underwent open surgery, found no statistically significant difference in cancer control, urinary function or sexual function between the two types of surgery.
Critics of the OHTAC report say the Australian study has profound shortcomings – namely, that it compared the work of an experienced open surgeon to that of a robotics novice.
The study also reported outcomes only three months after surgery, which could mask longer-term benefits of the robotic approach, said Stephen Pautler, a professor of surgery at Western University in London, Ont., who was among the urologists who asked to have their names taken off OHTAC's final report.
"We said you [OHTAC] are basing the entire economic analysis on a flawed study," Dr. Pautler said. "They were absolutely rigid and would not change their mind."
(Intuitive, for its part, said in an e-mailed statement there are many studies backing the da Vinci Surgical System that rely on "real-world evidence." The company called OHTAC's heavy reliance on randomized controlled trial data "inconsistent" with recent health-technology assessments in other places, including Alberta, the only province that funds robot-assisted surgery.)
But Anthony Adili, the chief of surgery at St. Joseph's Healthcare and a cheerleader for robotic surgery, said he couldn't fault OHTAC when the committee had so little high-quality evidence at its disposal.
"We need to wear some of that blame," Dr. Adili said. "We have to work with our partners, including government and bodies like OHTAC, to say, 'Where is the data lacking and how can we look at this in a more rigorous way?'"
Dr. Adili, Dr. Shayegan and their colleagues at the Boris Family Centre for Robotic Surgery – named for the founders of Mountain Cablevision, who donated $10-million to fund the centre – run a research program designed to produce high-quality evidence on robotics.
For now, hospitals who want to keep their da Vinci robots running will have to squeeze extra money out of their tight global budgets, or rely on charity.

Dr. Bobby Shayegan speaks to a patient just before undergoing a robotic prostatectomy on Thursday, July 27, 2017. Often, donations cover the extra cost of a robot-assisted surgery in Ontario.
Christopher Katsarov/the Globe and Mail
Just last month, Vancouver General Hospital announced with fanfare that it would be getting a new da Vinci surgical system, thanks in part to a $1-million gift.
The new robot is a replacement for "Jack," named for Jack Poole, the late businessman whose $3-million donation helped pay for the original machine in 2007, and helped cover the cost of its first 500 procedures.
When the charitable money ran out, Vancouver General Hospital turned to an unconventional source to make up the funding shortfall: patients.
Beginning in August, 2011, the hospital asked patients who chose robotic surgery over the conventional kind to pay $2,814 to cover half the incremental cost of their surgery. Less than a year later, it began asking patients to cover all of the incremental cost – $5,628 a procedure.
Most of that money went to pay for the disposable instruments at the end of the da Vinci's arms, which cost thousands of dollars (the price fluctuates depending on the instrument and the exchange rate) and have to be replaced every 10 uses.
Larry Goldenberg, a professor of urologic sciences at the University of British Columbia who has performed nearly 700 robot-assisted prostatectomies at Vancouver General, said the out-of-pocket cost didn't deter prostate-cancer patients.
"You have to think about patient satisfaction," he said. "That's where these other advantages come in: Things like getting back to work sooner, returning to full activity, number of diapers used. … If I say there's a higher chance that you will be out of diapers within three months, versus six months or a year, which would you choose?"
In all, 212 patients paid for robotic surgery at Vancouver General before the practice was halted in early 2015, more than a year after Health Canada warned the British Columbia government that asking patients to pay part of the cost of an insured service violated the Canada Health Act.
Now, the hospital is covering the extra cost out of its global budget.
Health Canada's kiboshing of Vancouver General's payment model means patient pay is off the table everywhere else.
Vancouver General is the only hospital in British Columbia with a da Vinci system. Calgary, Edmonton, Montreal and Quebec City all have at least one surgical robot.
The rest are in Ontario, where, in most cases, philanthropic funds are covering the extra operating costs.
Proponents of robot-assisted surgery had hoped the Ontario Ministry of Health would eventually step in, which is unlikely after the OHTAC recommendation.
Peter Pisters, a cancer surgeon and president of the University Health Network, said public funding for robotic surgeries ultimately comes down to whether patients believe it is important to have "a handful of facilities in the province that offer world-class care."
"Is that a must-have or is that a nice-to-have?" Dr. Pisters asked. "If we believe that's a must-have, then robotic surgery must be part of that."
MORE FROM THE GLOBE AND MAIL: