
Diane Chênevert with son Philippe – who was born in 2000 with severe cerebral palsy – at the Centre Philou in Montreal in 2019.NathB/Handout
From the time Diane Chênevert’s son Philippe was born in 2000 with severe cerebral palsy he was treated by a co-ordinated group of specialists at CHU Sainte-Justine children’s hospital in Montreal.
As a quadriplegic with an intellectual disability, severe epilepsy, respiratory problems and other conditions, Philippe requires 24-hour care, primarily at home.
At CHU Sainte-Justine, his medical care was co-ordinated by his pediatrician and physiatrist who managed his other specialists, including gastroenterologists, cardiologists, respirologists, neurologists and urologists. That was until he turned 18 and, legally an adult, Philippe was transitioned into the adult health care system.
But Ms. Chênevert would not call the transfer of care a transition. “Nobody actually sat down and talked to me about a transition,” she said.
Health care systems for adults with complex medical conditions, particularly for those that arise at birth, are not as co-ordinated as those for pediatric patients. Five years after the transition, Ms. Chênevert said Philippe still does not have a physiatrist, gastroenterologist, cardiologist or urologist.
Through the care of comprehensive pediatric health care teams, young people with complex conditions like Phillipe’s are increasingly living longer, revealing large gaps between the two worlds of health care. Physicians who mainly treat adults are now caring for patients with conditions primarily treated by pediatricians, such as severe cerebral palsy, cystic fibrosis and sickle cell anemia. Advocates are pushing for changes in the fragmented adult health care system to better reflect the more centralized complex care teams in the pediatric world.
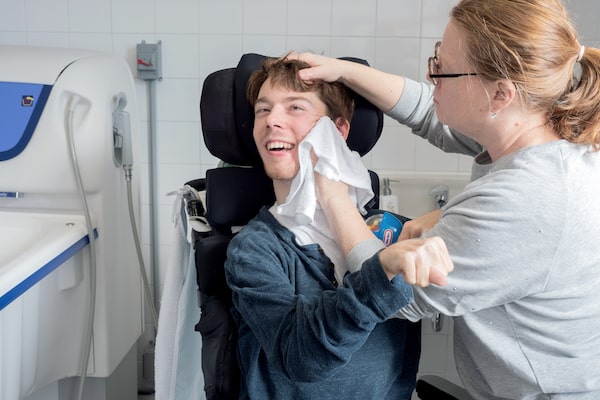
Ms. Chênevert began the Centre Philou to provide continuous and respite care and developmental services for poly-impaired children like Philippe.NathB/Handout
Many pediatric systems in Canada use a “head to toe” approach, said Dr. Sara Long-Gagné, the director of the Intermediate-Complexity Coordination and Navigation Service at the Montreal Children’s Hospital. These dedicated multidisciplinary teams offer a “one-stop shop,” enhancing communications between services within the hospital and communities while accommodating families through different phases of the child’s health.
“The care is more accessible and at the end of the day, we have an assessment, we have a plan and we can follow up,” Dr. Long-Gagné said.
Across Canada’s 13 children’s hospitals, there are established programs and policies to help young people have successful transitions into adult health care systems and empower them to take their care into their own hands. But these programs are designed to transition youth with less complex chronic conditions who do not require constant medical care from a variety of specialists.
In the decade Dr. Long-Gagné has worked as a pediatric complex care specialist, the number of children with complex medical conditions has increased and so has the number of medical complexities they have as these patients live longer.
The transition into the more fragmented adult health care system can pose risks, Dr. Long-Gagné said, including greater chances of medical errors, increased hospitalization complications and a more likely chance of emergency room visits or occupying hospital beds.
“It’s basically adding to the stress of the already very stressed health care system,” as well as adding stress to families and caregivers, Dr. Long-Gagné said.
Marcy White has been reluctant for her son, Jacob Trossman, to leave Toronto’s Hospital for Sick Children, known commonly as SickKids. Jacob has a rare neurodegenerative disease, and requires 24-hour care.
SickKids is preparing to transition Jacob, now 21, to the adult health care system in September after having extensions to stay through the pandemic. Ms. White has not found physicians with the same available resources or knowledge of Jacob’s care needs and has asked SickKids to allow him to stay for the remainder of his life.
“When you have a child like Jacob, it comes down to picking your battles. This is one that for me and for our family, we truly believe that Jacob’s life is at stake, that he will not get the type of care that he needs,” Ms. White said.

Ms. Chênevert has developed a plan – the first of its kind in Canada – to create a medical team to care for medically complex individuals from birth to end of life.NathB/Handout
In a statement from SickKids spokesperson Sarah Warr to The Globe and Mail, for medically complex patients requiring multiple specialists, the “SickKids Complex Care Program is a unique pediatric program that co-ordinates their comprehensive care needs.”
“There are no equivalent programs for young adults with medical complexity within a single adult hospital in Ontario,” Ms. Warr said.
Other parents have faced the challenges of transitioning out of complex care. Janice Carcone’s 20-year-old daughter Erin has a form of congenital muscular dystrophy and requires 24-hour care. She was transitioned from her team of 15 neuromuscular specialists at SickKids in January, 2020, and Ms. Carcone has struggled with the differences in care between the two systems.
Recently Erin was hospitalized for respiratory problems and Ms. Carcone said she brought in her own nursing staff to watch over Erin before they were sent home with oxygen instead of returning her to baseline level.
“We don’t want to end up in emergency departments. We have the nursing, we have the equipment in our house, we are able to handle a lot, but we do need the coaching from people who know what they’re doing,” Ms. White said.
Ms. Chênevert left her job in 2005 after 22 years in the aerospace industry and began her charitable organization Centre Philou, to provide continuous and respite care and developmental services for poly-impaired children like her son. Over the years, the organization has grown to encompass more than 200 children and young adults.
With investment from Deloitte and support from experts at the University of Montreal’s Centre Hospitalier, Ms. Chênevert has developed a plan to create a medical team to care for medically complex individuals from birth to end of life. It would be the first of its kind in Canada.
Ms. Chênevert said their plan shows that creating complex care teams in the adult care system could reduce the financial burden on the rest of the system by reducing emergency visits and creating a way for caregivers to receive medical advice at home.
“It’s putting a team together,” she said. “It just needs a lot of ambition, a lot of goodwill and looking to a new way of doing things, looking to solve the problem.”
 Joy SpearChief-Morris
Joy SpearChief-Morris