
Melody Cooper, 41, poses for a photograph in the Downtown Eastside in Vancouver. Ms. Cooper, who has been using drugs since she was 27, is now receiving hydromorphone and says it has changed her life.
DARRYL DYCK/FOR THE GLOBE AND MAIL
Melody Cooper throws a purple ball across the well-worn grass at the East Vancouver dog park, sending her dog, Squeak, bounding across the field. The Jack Russell-poodle cross is wearing a camouflage coat, pulled taut by a belly that jiggles with each bound.
"I didn't realize how much weight he had gained until recently," Ms. Cooper says, watching the dog from her seat on a park bench. "My mother pointed it out. She said, 'Look at him: When he lies on his side, two of his feet are still dangling in the air.'"
She smiles, breathing in the crisp winter air. Life these days is decidedly calmer for Ms. Cooper, who is one of just 30 people in Canada using hydromorphone to treat her long-time addiction. A recent Vancouver study found the pain medication to be an effective replacement therapy for an opioid dependency and, outside of the clinic where that study was conducted, she is the first person to receive the treatment.
It has turned her life around, she says.
More than 900 people died of illicit drug overdoses in this province last year – the highest such death toll on record. The powerful synthetic opioid fentanyl was confirmed in around 60 per cent of these deaths, and carfentanil – an animal tranquilizer many times more toxic than even fentanyl – is suspected in a recent surge of overdose deaths.
In neighbouring Alberta, new statistics released this week showed 343 illicit drug deaths were linked to fentanyl last year; the number of total illicit drug deaths is not yet available. Carfentanil was also detected in 22 of the 343 deaths.
The public-health crisis has spurred a far-reaching discussion on the public-health response. While some jurisdictions are just starting to equip first responders with naloxone, or are still debating the efficacy of supervised injection sites, others are looking beyond stop-gap measures to identify bold new interventions and regulatory changes.
The Globe and Mail spoke with health officials, addictions physicians, drug users and others about the next steps being contemplated – and the hurdles that remain.
Suboxone and methadone
The recently-formed BC Centre on Substance Use (BCCSU) this week released new guidelines for treating opioid dependency – the first comprehensive provincial document to guide care providers through the full scope of medical and psychosocial interventions available to treat opioid dependency. The guideline recommends against withdrawal management alone, which has been linked to elevated rates of relapse and fatal overdoses due to loss of tolerance. It reaffirms buprenorphine-naloxone, commonly referred to by its trade name, Suboxone, as the new first-line treatment for opioid dependency, as it is safer than methadone.
The guideline also places an emphasis on providing treatment options that meet people where they are at: Those who want to stop using as soon as possible, for example, should be placed on Suboxone or methadone and tapered down over the course of at least one month, then connected with long-term addiction treatment to prevent relapse and associated harms.
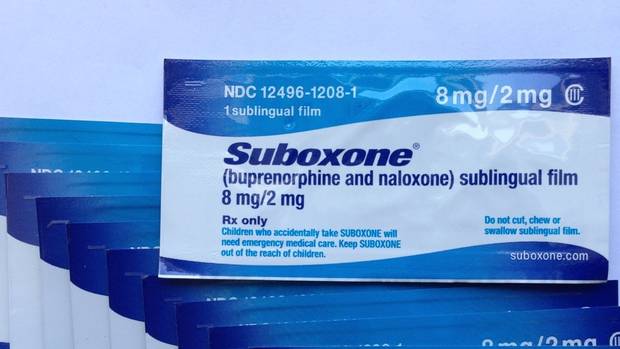
Suboxone, which has been proven effective to treat addiction.
As of Feb. 1, British Columbia's PharmaCare began covering the
full cost of Suboxone for those who make less than $42,000 a year.
Hakique Virani, a public health and addictions medicine specialist at the University of Alberta, says emergency departments should seize the opportunity to initiate treatment with Suboxone when people are taken to hospital for overdoses, or in opioid withdrawal.
"We know that patients who have had a non-fatal overdose are highly likely to have subsequent overdoses, including a fatal one," Dr. Virani said. "They are also very likely to use emergency medical services repeatedly. It is better medicine and better stewardship of resources and it is more humane to offer treatment at every touchpoint the patient has with the system."
In Vancouver, St. Paul's Hospital and a mobile medical unit temporarily stationed in the Downtown Eastside both have the capability to provide rapid access to various addiction treatments, including Suboxone. However, such treatment on demand is rare.
Heroin-assisted treatment
Heroin-assisted treatment (HAT) is an option for people who have failed repeatedly with traditional therapies such as methadone or Suboxone – an estimated 5 per cent to 10 per cent of all people on substitution treatment. This population is the most vulnerable and incurs the largest societal costs.
The North American Opiate Medication Initiative (NAOMI) out of Vancouver found that providing these people with pharmaceutical-grade heroin to be administered under medical supervision results in physical and mental-health improvements, reduced illicit drug use and reduced criminal activity.
In a 2013 report commissioned by Health Canada, Dr. Michael Lester, an expert in opioid dependence treatment, described HAT as "a promising treatment of last resort" for this population, noting there is no other "next step" for people who have failed multiple attempts at conventional substitution therapy.

A man identified only as Spike injects diacetylmorphine at the Providence Health Care Crosstown Clinic in the Downtown Eastside in Vancouver.
DARRYL DYCK/FOR THE CANADIAN PRESS
HAT has been available for years in several European countries, including Switzerland, Germany and Denmark. But in Canada, only 92 people – all former participants of the clinical trial – are receiving the treatment.
The hurdles that exist are not governmental. Federal Health Minister Jane Philpott supports the treatment and in September overturned the previous Conservative government's ban on it.
But because pharmaceutical-grade heroin is not manufactured or marketed in Canada, physicians must access it through Health Canada's Special Access Programme (SAP), submitting an application for each prospective patient. If approved, the drug then has to be imported from Switzerland – a process that can be prone to delays – in shipments containing no more than six months' supply at a time. Physicians must resubmit these applications, for every patient, every six months.
Last month, Dr. Philpott wrote to provincial and territorial health ministers noting that clinical evidence supports unconventional treatments such as pharmaceutical heroin, and that Health Canada's chief medical adviser is available "to further explore with your officials what they anticipate the needs are and any potential obstacles to accessing needed treatments."
Providence Healthcare estimates one person using illicit opioids costs society around $48,000 a year in health-care and criminal-justice costs. In comparison, it costs about $25,000 to put a person on HAT for one year at the Crosstown Clinic.
Hydromorphone
A follow-up study to NAOMI, the Study to Assess Long-term Opioid Maintenance Effectiveness (SALOME), found that hydromorphone, a licensed pain medication, is as effective a replacement therapy as pharmaceutical-grade heroin. It's a particularly attractive option as it is already available in Canada and does not have the stigma of heroin.
At present, 27 people who participated in SALOME remain on injectable hydromorphone at the Providence Crosstown Clinic, along with one new patient who started in August. Christy Sutherland, an addiction medicine specialist and medical director of the PHS Community Services Society, has also separately started two of her patients on injectable hydromorphone – including Melody Cooper.
Ms. Cooper had been a patient of Dr. Sutherland's for many years and had tried methadone, Suboxone and detox numerous times. Nothing worked. Dr. Sutherland feared her patient would die.
When the physician read the SALOME research paper, she immediately thought of Ms. Cooper.

Registered Nurse Tim Parizeau, left, administers a dose of hydromorphone to Melody Cooper.
DARRYL DYCK/FOR THE GLOBE AND MAIL
In September, Dr. Sutherland started Ms. Cooper on injectable hydromorphone.
"It was just amazing," Dr. Sutherland said. "She hardly missed a dose and she has stopped using. She doesn't meet the criteria for substance use disorder anymore."
Ms. Cooper says the change has been drastic.
"Now my life is so happy and relaxed," she said. She now works two part-time jobs – cleaning and peer support at the clinic in her residence – and returned to her old hobbies: beading, painting and origami.
"I don't even have the cravings anymore. I'm not out there trying to find my next fix, not risking my life or going to jail. I'm not one of those people overdosing on fentanyl."
There are no regulatory hurdles preventing a physician from starting a patient on hydromorphone as a substitution therapy. Hydromorphone is licensed as a pain medication, which would make its use as an addiction medication off-label, but this is permitted by the College of Physicians and Surgeons of B.C. so long as there are compelling reasons and the physician has an informed consent discussion with the patient, said registrar Heidi Oetter.
It costs about the same to put one person on supervised injectable opioid assisted treatment with hydromorphone at Crosstown as it does with heroin: roughly $25,000 a year.
Decriminalization and legalization
In 2001, Portugal decriminalized the purchase, possession and consumption of all psychoactive drugs for personal use, defined as 10 days' worth for an average person. That legislation essentially formalized the country's existing emphasis on treatment over punishment for drug users, replacing criminal penalties with administrative penalties. Those found using appear before a local Commission for the Dissuasion of Drug Addiction, which then considers individual circumstances and can impose a noncriminal sanction such as a referral to treatment or a monetary fine. It remains illegal to manufacture, sell and distribute drugs.
Three population surveys since 2001 suggest drug use increased slightly, but then fell to rates lower than before the legislation was enacted. Drug deaths plummeted; a 2016 report by European Monitoring Centre for Drugs and Drug Addiction found that fatal overdoses fell to levels among the lowest in the European Union, as did new cases of HIV and AIDS among drug users.
In British Columbia, top health officials, including provincial health officer Perry Kendall, have voiced support for decriminalization. Patricia Daly, chief medical health officer and vice-president of public health for Vancouver Coastal Health, said she supports not only decriminalization, but full legalization, which would entail state regulation of production, sale and use. Unwanted adulterants, such as deadly fentanyl and carfentanil, would be obsolete in a regulated market.
Asked about the issue in a November interview, B.C. Premier Christy Clark said she agreed addiction should be treated as a health issue but declined to support decriminalization.
"I think we might differ because I know that [Dr. Kendall and Dr. Daly] do support the legalization of a broad range of drugs and I don't want to end up in that category, because I'm not," the premier said. "But I absolutely agree that we need to treat addiction as a health issue because people who are addicted need their health, and their mental health, issues addressed and jail is often not the best place to do that."
Dr. Philpott, the health minister, interviewed on the subject in January, said drug policy is a sensitive topic for many but that "we are at the point we do need to talk about all the possibilities."
Asked if a Liberal government would consider decriminalization, the minister said it may not necessarily be the best route to go.
"If you look to cannabis, on the recommendations of the authorities, and recognizing the role of organized crime," she said, "we felt that it was not appropriate to simply decriminalize, that the right step to do was go to a strict regulatory regime with restrictions for access."
Donald MacPherson, executive director of the Canadian Drug Policy Coalition and former drug policy co-ordinator for the City of Vancouver, said regulation must be embraced as the next step in harm reduction.
"That is the stated objective behind cannabis regulation: They're doing this to protect youth, they're doing this to protect public safety," Mr. MacPherson said. "The same argument applies to all other drugs, as difficult as that is to put forward. We need to get beyond the point where we're afraid of that, because what we have now is absolutely not working."
MORE FROM THE GLOBE AND MAIL:

