
Vincent Lam stands outside a Toronto pop-up vaccination clinic. Dr. Lam has been administering COVID-19 shots for the past month whenever he's not busy with his usual addiction-medicine clinic.Photography by Fred Lum/The Globe and Mail
Vincent Lam is an author and a physician. He is the Medical Director of the Coderix Medical Clinic. Currently, he is assisting with the COVID-19 vaccination efforts of Michael Garron Hospital, Toronto Public Health, and Unity Health.
I gently massage the shoulder of the patient, drop my voice to say, let your arm fall, and the deltoid muscle relaxes between my thumb and forefinger. A tense arm becomes loose, as if letting go after a year of hanging on tightly. Mid-squeeze, I slip in the needle, and inject less than a millilitre of vaccine. The patient says, surprised, that the shot was not painful, “That’s it? Are you done already?” Perhaps there is a sense of anticlimax. After a year of COVID-19, after enduring months of political bluster and collective angst surrounding vaccine rollout with too few doses to be had, after running the gauntlet of booking a vaccine appointment, the patient sees that I am already taping a cotton ball to their arm. “I didn’t even feel it,” many say. It may be the thin gauge of needle, but when patients compliment me on technique, I accept graciously. I say with a flourish, like a proud child who has learned a magic trick, “I’ve been practicing.”
Muffled by a mask, vision blurred by a plastic shield, I work at a small table draped with plastic, folding chairs on either side, among a dozen other vaccinators seated in rows. I am armed with alcohol swabs, cotton balls, medical tape, disinfectant wipes and a pump bottle of sanitizer. Laminated signs allow me to communicate with co-workers, including the pharmacy team behind nearby curtains who prepare vaccine, which are despatched by runners to myself and the other vaccinators in small batches throughout the day.
Hoping that this moment will be memorable, I provide caveats immediately after the shot: that it takes a few weeks to develop the greatest immunity from the vaccine, which is only one tool among other public health measures, that data is still evolving on the effectiveness of our vaccines against the new variants of COVID-19, that we are in the third wave, and therefore all public health guidance should continue to be followed despite the jab: distancing, masking, outside is safer than inside. It is like standing at the finish line of an ultraendurance race, an extreme event in which the runners have been at it for over a year, with fear and boredom as their companions. And now you have arrived! The finish line! The shot! And by the way, you have to keep on running! But hopefully with less fear.
Over the past month, when not in my usual addictions medicine clinic, I have been administering COVID-19 vaccines. To the question many of us have asked during this pandemic, what can I do to help? this is my answer as one physician, one citizen. This work has taken me to convention centres, long-term care homes, apartment buildings, homeless shelters, community centres and a tent in a school parking lot outside of which people queued for four hours in near-freezing temperatures.
One woman bounced toward me, exclaiming, “I am so happy and excited. Is everyone this excited?” Many are eager. A few are apprehensive. There is often some mix of relief, exhaustion, triumph, resignation, the emotional sediment of the past year distilled into this moment.
Some people tell me of a relative who has succumbed, or recovered, or is currently in an ICU struggling with COVID-19. For everyone, the past year has been dimmed with the sadness of lost human interactions. Grandparents tell me they want to see their grandchildren. Some, with walkers or a cane, are assisted by a family member who tells me this is the first time they have left the home in a year.
Others want to get something off their chest before I tell them what to expect with the vaccine – their frustration with acquaintances who flout public health guidelines, anger with the political handling of the pandemic, anxiety regarding the delayed second dose. I commiserate, because I may be a physician, but I have also felt tiny as large events unfold around me. I also have my criticisms of our political leaders. I am also waiting for my second shot.
Some pull up their sleeve as they approach, offering me a bared shoulder for the jab before I have even had a chance to say hello, never mind review contraindications and obtain informed consent. It is as if they are saying without words, I’ve heard enough. Everything has been said. Just do it.
Before giving the vaccine, I deliberately emphasize to each person what to expect in the next two days: sore arm, tiredness, headache. I say “If these happen, it is your body reacting to the vaccine. We want it to react to the vaccine.” In this framing, I hope to transform discomfort into reassurance. It feels crucial to tell people what to expect, as the past year was suffused, for many of us, with the anxiety of not knowing what was about to happen.
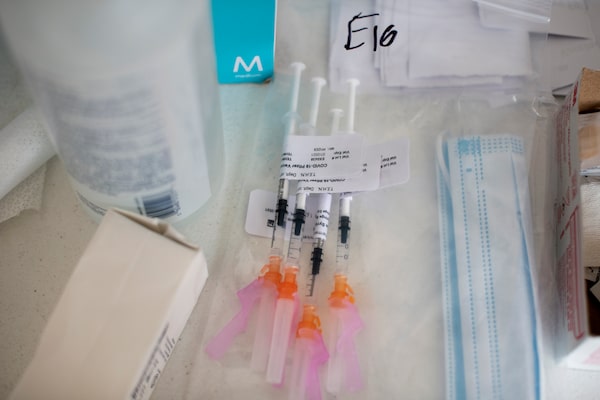
Syringes filled with the Pfizer-BioNTech vaccine are ready for use at the pop-up clinic.
As I slip each shot into each arm, I am aware of being in the calm centre of an out-of-control COVID-19 storm. Outside, daily case counts soar. ICUs are bursting. Hospitals overflow into tents. Police are posted at Ontario’s borders. Meanwhile, in my role as a vaccinator, I seek comfort in ritual and repetition – checking that the hub of the needle is tight on the barrel of the syringe lest it leak and the precious dose be wasted, inspecting for stray air bubbles and coaxing them out of a syringe, wiping and sanitizing between each interaction – over and over again. Many patients want a selfie of the moment when my needle enters their arm. I encourage them to share photos on social media – tell everyone that this is possible, and essential.
Outside of my days spent vaccinating, I am still running my addictions clinic, where COVID-19 has poured gasoline on the raging fire of opioid overdoses and death. My friends from the emergency department where I previously worked during SARS tell me that a third of the patients they are now seeing have COVID-19. My wife is covering an inpatient unit that has been converted overnight into a COVID-19 unit, where patients are being admitted with the variant strains of virus.
Some of my most vulnerable addictions patients have been vaccinated through shelters, but not all. Some were confused about the date of the vaccine outreach. Others I tried to persuade, but they declined the vaccine. However, many of my patients – food industry and service workers, our essential heroes who infuriatingly were not given paid sick days in Ontario until Doug Ford’s government was shamed into doing so by its political opposition, unions and doctors – are keeping us all fed, while anxiously hoping and scrambling for a vaccine.
Tantalizingly, the Centre for Addiction and Mental Health in Toronto began to offer vaccines to anyone with a diagnosis of a substance use or mental health disorder but, predictably, with one in five Canadians in any given year experiencing a mental health or substance use disorder, and this figure worsening as the pandemic drags on, demand far outpaces supply at their CAMH vaccine clinic. Every single one of my patients legitimately qualifies under this criteria, although many have put their substance-use demons to rest and see me for continuing maintenance care. Most live in priority postal codes.
In my addictions clinic, the patient sits at a distance from where I am perched at my computer while I click open more browser windows trying to book a vaccine appointment for them. As many know, the systems are not intuitive. I click my way past screens that warn that no vaccines will be given without an appointment, find a calendar that offers hope, and thus far – have always reached a dead end. No appointments available. While on my vaccination days, I spend hours doing nothing but giving shot after shot, when I am outside of that system, all I can do is sheepishly tell my patients that they should check often, that they need to be lucky and quick to book when the next spots are released.
In the vaccination centres, I struggle to be heard through a mask, a face shield, and the din of the steady stream of COVID-19 distanced people. I shout, and the patient on the other side of the Plexiglas shield shakes their head, points at their ear. I can see that they are also shouting, and I can barely make them out. This is like so much of the pandemic, so many of us isolated, yelling to get through, muted by a virus.
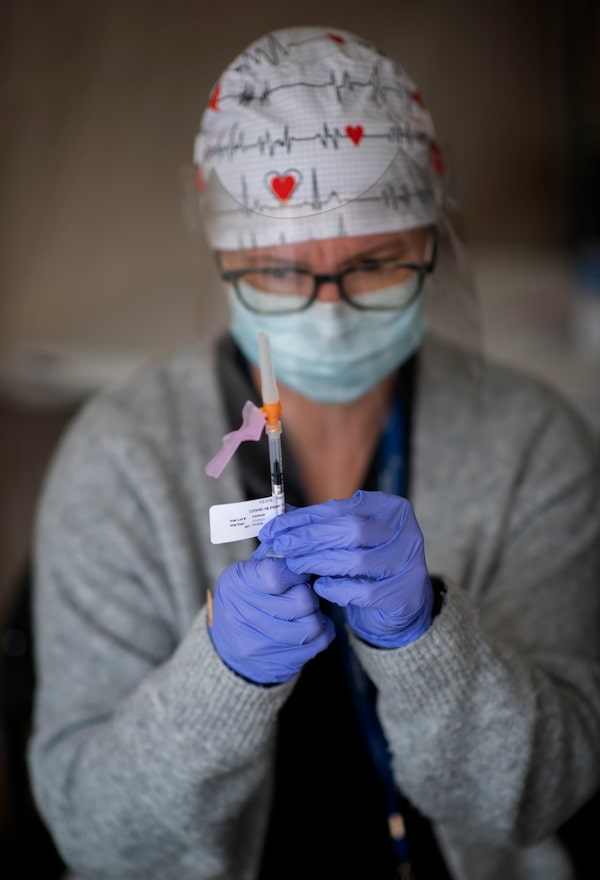
Nurse practitioner Candice Sockett prepares a dose of a COVID-19 vaccine at the pop-up clinic.
In my clinic, more of my patients meet the age criteria for vaccination as the threshold falls. When I ask, some have already received the shot, but some eligible patients are undecided, wary. I ask, “Do you have any questions about vaccines?” When my patient has a specific question, about blood clots, or about how the vaccines were developed so quickly, I answer as eagerly as a medical student who has just read a textbook.
Others do not have a specific query. Following a year during which health guidance necessarily shifted many times in response to emerging knowledge and the evolution of the pandemic, but often changed amid controversy and discord, some people are simply slow to trust. I hear, “First they say to get this shot. Then I hear about blood clots. What will they say next week?” Despite me giving it my best, trying to humanize statistics and risk-benefit concepts, the reply I receive is, “There’s just a lot of stuff out there … I’ll keep an eye on it,” as if they are being picky about umbrellas while unconcerned that a hurricane approaches.
A number of people tell me with a tone of almost strident satisfaction that they will not take a shot. I wonder if, after a year of being told what to do, this refusal is an opportunity to be in charge of something. Whether it is suspicion, an unformed disquiet, or outright rejection of the vaccine, I need to restrain myself from shouting as I do when I am in a vaccination centre. I want to yell, “For God’s sake, this is a miracle of modern medicine that could save you from a horrible death gasping for air! The last patient I saw desperately wants one, but we couldn’t find an appointment for their eligibility! I spent 10 hours yesterday jabbing as people as many as I could! What’s wrong with you?” This will not be useful, and instead I try to summon equanimity, saying, “It’s important that you are comfortable, and that you have good information. Can we talk more about vaccines next time I see you?”
While the keen science geek in me revels in having a small part in a global scientific triumph, giving massively effective and safe vaccines that have the potential to save millions of lives, working in the vaccination centres is repetitive and yet requires careful attention to detail. Reading about the vaccines is thrilling. To give them all day is to be a tiny cog. I am tasting the flavour of work that many warehouse, food-service, and other essential workers perform for years, the heroes who have kept our society fed and functioning over the past year with few of the benefits I enjoy as a physician.
To save my voice, which becomes more and more hoarse throughout the day, I try to streamline my questions and explanations, to hit key points with the least number of words possible. My back and neck ache from hunching over. By the fiftieth shot, I ask about allergies, and realize I have already asked. These are observations, not complaints. Like much of the pandemic, issues of global significance bear down upon each of our lives, and conversely our tiny individual actions ripple outwards like the stone dropped into water, the proverbial butterfly wing. It is numbingly repetitive to give shot after shot, just as it is to heed public health advice and to stay at home yet again, to remain distant from those whom we long to see and to embrace. It is lonely to not be heard, whether this is from shouting or from restraining oneself from shouting. This is true whether one is practicing medicine or just trying to make it through another week of the third wave, our lives our own but not fully under our control.
All of us want to celebrate the end of this period of our lives, our pandemic life, but that time – although it glimmers as a possible near future – has not yet arrived. So much hinges upon each of us, right now, paying meticulous attention to the monotonous, no matter how fed up we may be: distance, masks, outdoors. In this rare moment of exception, one of fleeting human contact, I wipe the skin over the deltoid with alcohol, squeeze the shoulder, feel the muscle release, give way, and then I plunge the needle.

Keep your Opinions sharp and informed. Get the Opinion newsletter. Sign up today.